general perspective
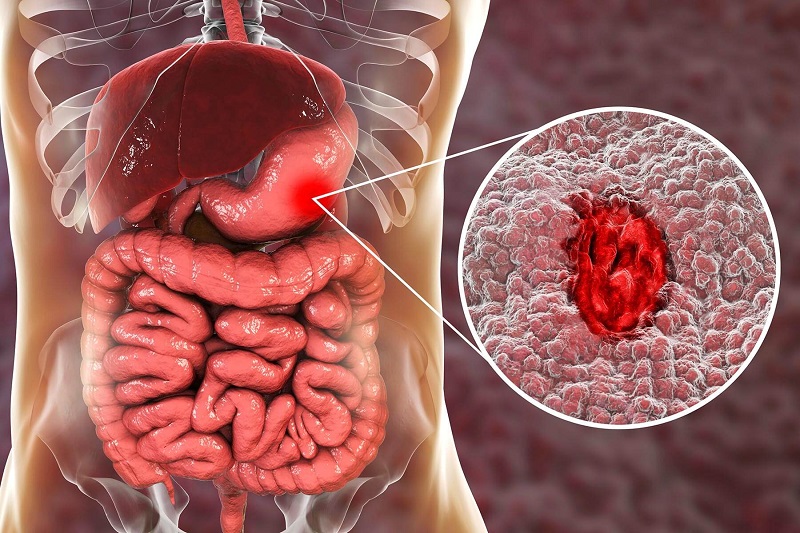
Peptic ulcers are sores that appear on the inner lining of the stomach and the upper part of the small intestine. The most common symptom is stomach pain.
Peptic ulcers include:
- Gastric ulcers that occur inside the stomach
- Duodenal ulcers occur inside the upper part of the small intestine (duodenum)
The most common causes of are infection with Helicobacter pylori (H. pylori) bacteria and long-term use of nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen (Advil, Motrin IB, others) and naproxen sodium ( Aleve). However, stress and spicy foods do not cause peptic ulcers but can worsen symptoms.
Symptoms
- burning stomach pain
- Feeling of fullness, bloating, or belching
- Intolerance to fatty foods
- stomach acidity
- nausea
The most common symptom of disease is burning stomach pain. Heartburn makes the pain worse, as does having an empty stomach.
Less commonly, ulcers can cause severe signs or symptoms such as:
- Vomiting or throwing up blood, which may look red or black
- Dark blood in the stool, or stools that are black or tarry
- Difficulty breathing
- feeling weak
- nausea or vomiting
- Unexplained weight loss
Causes
Peptic ulcers occur when acid from the digestive system eats away at the inner surface of the stomach and small intestine. The acid can create an open sore that is painful and may bleed.
The digestive system is covered by a mucous layer that usually protects it from acid. However, if the number of acids increases or the mucus decreases, you may develop an ulcer.
These are the most common causes:
- A bacterium Helicobacter pylori bacteria usually live in the mucosal layer that covers and protects the tissues lining the stomach and small intestine.
It’s not clear how Helicobacter pylori infection is spread. It can be spread from one to another by close contacts, such as kissing. People can also get Helicobacter pylori from food and water.
- Frequent use of certain pain relievers. Taking aspirin, like specific prescription and over-the-counter pain relievers called nonsteroidal anti-inflammatory drugs, can irritate or inflame the lining of the stomach and small intestine. These medications include ibuprofen naproxen sodium (Aleve, Anaprox DS, others), ketoprofen, and others.
- Other medications. Take certain medications, such as steroids, blood thinners, low-dose aspirin, selective serotonin reuptake inhibitors, alendronate (Fosamax), risedronate (Actonel), and nonsteroidal anti-inflammatory drugs, can significantly increase the chance of ulcers.
Risk factor’s
you may be at increased risk of peptic ulcers if you:
- Alcohol can irritate and eat away at the stomach’s mucosal lining, increasing the amount of stomach acid produced.
- You have untreated stress.
- You eat spicy foods.
complications
If left untreated, peptic ulcers can occur:
- Internal bleeding. The bleeding can occur as slow blood loss leading to anaemia or severe blood loss that may require hospitalization or a blood transfusion.
- A hole (perforation) in the wall of your stomach. this can perforate the stomach or small intestine wall, causing a severe abdominal cavity infection.
- Obstruction. Peptic ulcers can block the passage of food through the digestive tract, leading to bloating, vomiting, and weight loss, either from swelling from inflammation or scarring.
- Stomach cancer. Studies have shown that people infected with Helicobacter pylori have an increased risk of stomach cancer.
Prevention
You can reduce your risk of developing peptic ulcers by following the strategies recommended as home remedies for treating ulcers. It can also be helpful for the following:
- Protect you from infections. there is evidence that it could be passed from person to person or through the consumption of food or water.
- You can take precautions to protect yourself from infections, such as Helicobacter pylori, by washing your hands often with soap and water and eating foods that have been thoroughly cooked.
- Be careful with painkillers.
Avoid consuming alcohol when taking medications, as the combination of the two can increase the risk of an upset stomach.
Diagnosis
To detect an ulcer, first take your medical history and do a physical exam. You need to diagnostic tests, such as the following:
- Laboratory tests to detect Helicobacter pylori bacteria. Your doctor may recommend tests to determine if Helicobacter pylori bacteria are present in your body. You can look for it with a blood, stool, or breath test. The breath test is the most accurate.
- For the breath test, you eat or drink something that contains radioactive carbon. Helicobacter pylori bacteria break down the substance in the stomach. Then, you blow it into a bag, which is then sealed. If you are infected with Helicobacter pylori, your breath sample will contain radioactive carbon in the form of carbon dioxide.
- You should tell your doctor if you take an antacid before your Helicobacter pylori test. Depending on the test used, the medication may need to be stopped for a time because antacids can give false negative results.
- Endoscopy. The doctor may use an endoscope to examine the upper part of the digestive system (endoscopy). During endoscopy, the doctor inserts a hollow tube equipped with a lens (endoscope) down your throat and into your oesophagus, stomach, and small intestine. Using the endoscope, the doctor looks for ulcers. If any are found, a small tissue sample (biopsy) may be removed for examination in a laboratory. A biopsy identify the presence of Helicobacter pylori bacteria in the lining of the stomach. If the endoscopy shows a stomach ulcer, a follow-up endoscopy should be done after treatment to determine if it has healed, even if symptoms improve.
- Upper gastrointestinal series. Sometimes called a “barium swallow study,” this series of x-rays of the upper digestive system produces images of the oesophagus, stomach, and small intestine. During the x-ray, you swallow a white fluid (containing barium) that coats your digestive tract and makes an ulcer more visible.
- Endoscopy
An endoscopy involves inserting a long, flexible tube (endoscope) down your throat and into your oesophagus. endoscope allows the doctor to examine the oesophagus, stomach, and duodenum, where the small intestine begins.
Treatment
Treatment of peptic ulcers depends on the cause. Treatment will usually consist of killing the H. pylori bacteria if present, eliminating or reducing the use of nonsteroidal anti-inflammatory drugs, NSAIDs if possible, and helping the ulcer heal with medication.
Medications include the following:
Antibiotic medications to eliminate Helicobacter pylori. If H. pylori are found in your digestive tract, your doctor may recommend a combination of antibiotics to kill the bacteria. These antibiotics include amoxicillin (Amoxil), clarithromycin (Biaxin), metronidazole (Flagyl), tinidazole (Tindamax), tetracycline, and levofloxacin.
Antibiotics will be chosen based on where you live and current antibiotic resistance rates. In addition, you’ll likely need to take antibiotics for two weeks and additional medications to reduce heartburn, including a proton pump inhibitor and possibly bismuth subsalicylate (Pepto-Bismol).
Medications that block acid production and promote recovery. Proton pump inhibitors (PPIs) reduce stomach acid by blocking the action of the parts of the cells that produce acid. These medications include over-the-counter and prescription drugs such as omeprazole (Prilosec), lansoprazole (Prevacid), rabeprazole (Aciphex), esomeprazole (Nexium), and pantoprazole (Protonix).
Long-term use of proton pump inhibitors, especially at high doses, can increase the risk of hip, wrist, and spine fractures. Ask your doctor if a calcium supplement might reduce that risk.
Medications to reduce acid production. Acid blockers, also called histamine H2 receptor antagonists, decrease the amount of stomach acid released into the digestive tract, which relieves ulcer pain and promotes recovery.
Available over-the-counter and prescription acid blockers include drugs such as famotidine (Pepcid AC), cimetidine (Tagamet HB), and nizatidine (Axid AR).
Antacids that neutralize stomach acid. Your doctor may also add an antacid to your medication regimen. it neutralize stomach acid and can provide quick pain relief. Depending on the main ingredients, some side effects can be constipation or diarrhoea.
Antacids may relieve symptoms but are not usually used to heal the ulcer.
Medications that protect the lining of the stomach and small intestine. In some cases, doctor may prescribe medications called cytoprotective agents that help protect the tissues that line your stomach and small intestine.
Options include sucralfate (Carafate) and misoprostol (Cytotec), both prescription drugs.
Follow-up after initial treatment
Treatment for peptic ulcers is usually successful and usually allows the ulcer to heal. However, if your symptoms are severe or continue despite treatment, your doctor might recommend an endoscopy to rule out other possible causes.
If an ulcer is found during the endoscopy, your doctor might recommend another endoscopy after treatment to make sure the ulcer has healed. Ask your doctor if you should have follow-up tests after treatment.
Ulcers that do not heal
Peptic ulcers that do not heal with treatment are called refractory ulcers. There are many reasons why an ulcer might not recover, including the following:
- Not taking medications as directed
- The fact that some types of Helicobacter pylori are resistant to antibiotics
- Frequent use of tobacco
Less commonly, refractory ulcers may be the result of:
- overproduction of acid in stomach, such as occurs in Zollinger-Ellison syndrome
- An infection other than Helicobacter pylori
- Stomach cancer
- Other diseases that can cause ulcers in the stomach and small intestine, such as Crohn’s disease
The treatment of refractory ulcers usually consists of eliminating the factors that can interfere with recovery and using different antibiotics.
Today, however, the need for surgery is less frequent due to the availability of many effective medications.
lifestyle and home remedies
To ease the pain of a stomach ulcer, you can try the following:
Change painkillers. If you take pain relievers regularly, ask your doctor if acetaminophen (Tylenol, others) might be an option for you.
Controlling stress. Stress can make the signs and symptoms of a peptic ulcer worse. Think about the sources of your stress and do what you can to address them.
No Smoking. Smoking can interfere with the stomach’s protective lining, making it more susceptible to ulcer development. Smoking also increases stomach acidity.
Limit or avoid alcohol. Excessive use of alcohol can erode the mucosal lining of the stomach and intestines, leading to inflammation and bleeding.
alternative medicine
Products that contain bismuth can help with the symptoms of a peptic ulcer. For example, powdered mastic produced from an evergreen shrub may also help improve symptoms and speed the healing of peptic ulcers.